Teledermatology FAQs
Please refer to our frequentlyasked questions below:
- What is teledermatology?
Teledermatology involves referring an image of the skin or the skin appendages of a patient together with relevant history of the condition to a clinician for further review. A qualified professional will take a series of digital photographs of your skin lesion. These photographs will be sent to a dermatologist for remote assessment to see if you need to come into hospital for further review or treatment.
Your images may be taken by your Primary Care Team at your local GP practice or you may be referred by your GP to Vita Health Group, who will take the photographs at Ainsdale Health & Wellbeing Centre. Please note, only lesions that are documented on your referral can be photographed during your appointment.
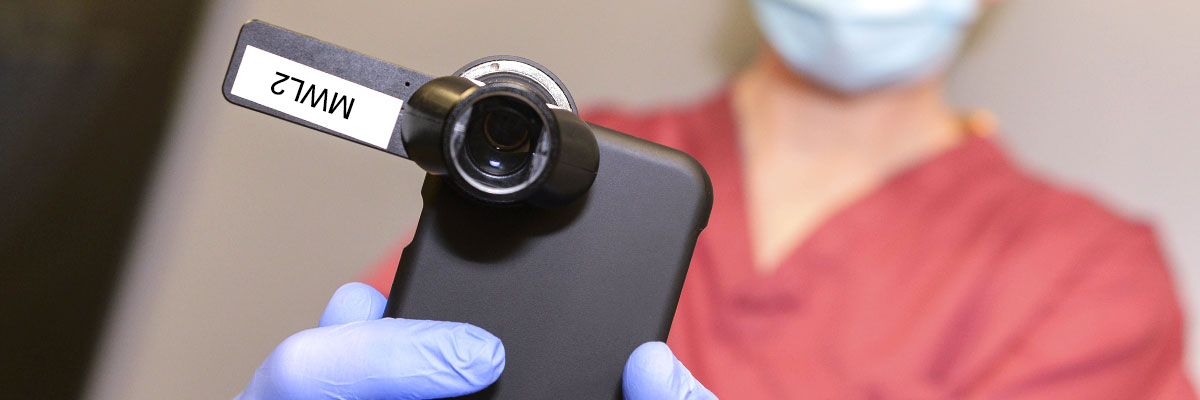
The photographer may use two different devices to take photographs:
- a camera phone, and
- a HEINE Delta-One Dermatoscope
They will photograph a general view of the area of interest to establish the location of your lesion, and a detailed close up using a specialised lens called a dermatoscope. The dermatoscope allows the photographer to capture highly detailed images of your lesion, by pressing gently against the surface of the skin. This should not hurt.
It may not be possible to photograph some lesions using the dermatoscope. This will be explained to you at your appointment. In these cases you will be referred directly for a face-to-face appointment.
Once the photography is complete, your images will be securely uploaded to Cinapsis, where they will then be reviewed by a Hospital Dermatologist. The Dermatology team will assess the clinical photographs. They will then contact you within 10 working days, to advise of the outcome.
If the Dermatology Medical Team concludes a hospital appointment is required, they will arrange for the hospital administration team to contact you for an appointment in a dermatology clinic (e.g., for face-to-face review or to take a small skin sample (biopsy), or removal of the lesion).
If the Dermatology Medical Team concludes you do not need to visit the hospital, your GP will be informed of the recommended action. This could be no action required, a recommendation to undertake further investigations, or advice to provide specific treatment.
A copy of the recommendations will also be sent to you by post.
If you are concerned about any other lesions or skin problems, please seek advice from your GP.
- How long will my appointment take and what will happen?
You will be asked a series of questions related to your medical history and specific details of the lesion itself. The photographer will explain what photographs need to be taken to assess your lesion before they proceed. If you have any questions about the photography, please do not hesitate to ask.
Please note you may be asked to remove jewellery or make up where necessary. Depending on the location of your lesion, you may also be asked to remove articles of clothing to gain a better view of the area of interest. If you are required to remove clothing, you may request a chaperone. This whole process will take approximately 20 minutes.
- Do I need to give permission for photographs to be taken?
Yes. The clinical photographer will discuss consent with you in detail to ensure you are comfortable with the photographs being taken and how your clinical images will be used. If you are happy to proceed, you will be required to provide verbal confirmation of your consent, which will be recorded on your referral form
We will not take any photographs without your permission.
You may withdraw your consent at any time by contacting the Hospital Dermatology department. Clinical photographs that have been used to make a clinical decision cannot be deleted, however your images can be retracted and hidden from view on your electronic patient record.
Retracting consent will not affect your treatment or any future treatment you may receive.
- How is my data used by Skin Analytics?
To process your assessment, Cinapsis will securely store your medical referral and images, together with standard identification information necessary for the safe and accurate filing of the assessment report (i.e. your name, date of birth and NHS number).
The assessment report will be available for MWL Trust to use appropriately in support of any further care or treatment you may need.
The results of the assessment will be sent to your GP practice to be included in your medical records.
More information on how the Trust processes your data can be found on the Trust website - https://www.merseywestlancs.nhs.uk/mwl-privacy-statement
- What happens after my photographs have been reviewed?
After reviewing your photographs, the dermatologist may offer you further treatment and contact you and your GP with a letter about your lesion management or offer you a face-to-face appointment.
- How will I find out the result of this photographic procedure?
You should receive a letter in the post within a maximum of ten working days of your referral or a telephone call asking you to attend a face-to-face consultation.
If you have not been contacted by the hospital with the outcome of your clinical review within ten days of the date of the request, please contact the dermatology team on 01695 656 115 between 09:30 – 16:00, Mon-Fri. If outside of these hours, please leave a message and the team will contact you urgently.
If an outcome cannot be determined you may be asked to:
- book a biopsy (skin sample) or the removal of the skin lesion
- book a priority face-to-face clinical appointment with a dermatologist in hospital
If you require non-urgent treatment, the Dermatology team may
- contact your GP to arrange treatment for you
- refer you to Vita
- Does an urgent follow up appointment or surgery mean I have cancer?
No. You could be asked to come back urgently for a number of reasons. Urgent appointments will generally be seen within a few weeks, so there should not be a long wait.
- Can I have copies of the photographs?
You have the right to access the information we hold about you, such as your medical information. Requests must be made in writing to the Access to Medical Records department.
The Trust will provide your information to you within one month from receipt of your application. This can be extended dependent on the complexity of the request.
Please note that some or all of the information requested may be withheld in reliance on exemptions contained within the UK GDPR and Data Protection Act 2018.
You must complete a request form to see your records using this form:
A copy of a form of photo identification is required for all access requests (e.g. passport, driving license NUS card). For all requests, a copy of a utility bill or bank statement no more than three months old will also be required to confirm address. You must provide your identity documents with the request form. (These will be destroyed once the request is closed.)
The application form and identification should then be sent to:
Access to Health Records
Mersey and West Lancashire Teaching Hospitals NHS Trust, Town Lane, Kew, Southport, PR8 6PN
Or
soh-tr.access-to-health@merseywestlancs.nhs.uk
If you require assistance, please call 01704 704616 or email soh-tr.access-tohealth@merseywestlancs.nhs.uk.
Access to records of a deceased person
Records of the deceased are governed by the Access to Health Records Act and are usually kept for eight years after the patient’s death.
Only the person with an absolute right of access is the personal representative, who is the executor or administrator of the deceased persons’ estate.
Other individuals with a claim may request information and will be required to define on what grounds the request is being made.
- When should you worry about a mole?
It is important to check your skin regularly for any change. You may want to ask a family member or a friend to examine your back.
Following the ABCDE – easy rules can help you identify potentially worrying features:
- Asymmetry – the two halves of the lesion may differ in shape
- Border – edges of the lesion may be irregular, blurred or notched
- Colour – the colour may be uneven
- Diameter – report any mole larger than 6mm or a change in size or shape
- Evolution – changes in size, shape, colour or elevation or any new symptom such as bleeding, itching or crusting
It can be helpful to take images of your lesion to see if the lesion is changing over time as it can be more reliable than using memory alone. It can be useful to do this every few months using a phone with a camera.
If you notice any of the changes described above or are concerned about a mole or patch of skin for any other reason then contact your GP as soon as possible.
- How can you reduce your risk of skin cancer?
It is recognised that unprotected exposure to UV radiation can increase your risk of skin cancer. It is therefore important to be careful in the sun.
The British Association of Dermatologists (BAD) have compiled the following ‘Top Sun Safety Tips’:
- Protect your skin with adequate clothing, wear a hat that protects your face, neck and ears, and a pair of UV protective sunglasses
- Choose sun protective clothing (with permanently sun-protective fabric, widely available for adults and children) if you have fair skin or many moles
- Spend time in the shade between 11:00am to 3:00pm when it’s sunny
- Step out of the sun before your skin has a chance to redden or burn
- When choosing a sunscreen look for a high protection SPF (current recommendations are SPR 50 or 50+) to protect against UVB, and the UVA circle logo and/or 4 or 5 UVA stars to protect against UVA
- Apply plenty of sunscreen 15 to 30 minutes before going out in the sun, and reapply every two hours and straight after swimming and towel-drying
- Keep babies and young children out of direct sunlight
- Sunscreens are not an alternative to clothing and shade, rather they offer additional protection (no sunscreen will provide 100% protection)
- Do not use sunbeds
