Delivering your baby
Location level 4, Ormskirk hospital
Our purpose-built delivery suite has eight delivery rooms and an obstetric theatre. Three of our delivery rooms are designated as active birth/midwifery led care rooms, with one of these rooms also having a birth pool.
The pool is available for women to use either as pain relief or for water birth. In addition if you specifically wish to labour in water we can facilitate the use of your own birth pool in one of our rooms. All the delivery rooms have en-suite facilities.
Telephone: 01695 656919
We make every effort to ensure your comfort and safety in our delivery rooms. As well as having state of the art monitoring equipment and birthing beds each delivery room has a sound system with docking station, CD player and radio.
The delivery suite is staffed by midwives and obstetricians who strive to ensure that the highest level of care and support is available for you before, during and immediately following the birth of your baby.
Your birthing partners will be made welcome, we recommend that you decide during your pregnancy who you would like to support you in labour and that you inform your midwife at your 36 week antenatal appointment of who you wish your birth partners to be.
We generally advise that you have up to two birth partners, however we are happy to support your personal choice if you feel you would need additional support.
Your community midwife is available to go over your birth plan with you at 36 weeks and on admission to delivery suite we welcome the opportunity to discuss your birth plan further.
Visiting the delivery suite
We do not have visiting times as visiting is usually open but restricted to your chosen birth partners. However, as birth is a significant and happy event for a family, we welcome short visits from baby’s grandparents and siblings following the birth.
If you need to remain on Delivery Suite following the birth of your baby we would ask that your visitors come from 2pm to 4pm and 6pm to 8pm.
- Fetal monitoring in labour
 Measuring your baby’s heart rate is a good way of checking their health and wellbeing throughout labour and birth.
Measuring your baby’s heart rate is a good way of checking their health and wellbeing throughout labour and birth.During labour when the uterus (womb) contracts, the maternal blood does not flow as freely through the placenta and this reduces the oxygen supply. This is a very normal process and most babies cope very well with this. However, if your baby does not cope as well with this then he/she might show signs in the pattern of the heart rate.
Methods of fetal monitoring
Before listening to your baby’s heartbeat, your midwife will perform a risk assessment at the start of your labour to determine the most appropriate way to listen to your baby’s heartbeat. Your baby’s heartbeat can be monitored either by intermittent auscultation (IA) or continuous cardiotocograph (CTG).
Intermittent auscultation (IA)
This method uses a Pinard stethoscope or handheld Doppler to listen to your baby’s heartbeat (similar to when your midwife has listened to your baby’s heartbeat during your antenatal checks). IA is most appropriate for labour and birth where the pregnancy has been uncomplicated.
During labour, your midwife will listen to your baby’s heartbeat for 60 seconds immediately following a contraction every 15 minutes in the first stage of labour and every 5 minutes in the second stage of labour (see your pregnancy information booklet for details on the stages of labour).

Throughout labour if your baby’s heartbeat is monitored by IA, there will be a regular review and discussion with another midwife (sometimes called Fresh Ears/Fresh Review) to ensure that IA is still the most appropriate method of monitoring for your baby and that your place of birth is still appropriate (e.g. home/pool). This discussion should include you and your birth partner, taking into account your wishes.
With IA you have the ability to move around, change positions easily and also access the birth pool if you wish to.
Continuous cardiotocograph (CTG)
This method uses a cardiotocograph (CTG) machine to continuously monitor and record your baby’s heartbeat throughout labour and birth and is usually advised when there have been complications in pregnancy (such as diabetes or reduced fetal movements) or if any observations carried out by the midwife are not within the normal range (such as a high pulse or temperature)
The CTG machine prints out your baby’s heartbeat on to a strip of paper, along with your contractions. This is done by applying two sensors to your abdomen, held in place by elastic belts. The midwife and/or doctor will “read” and interpret this monitoring to see how well your baby is coping with labour.
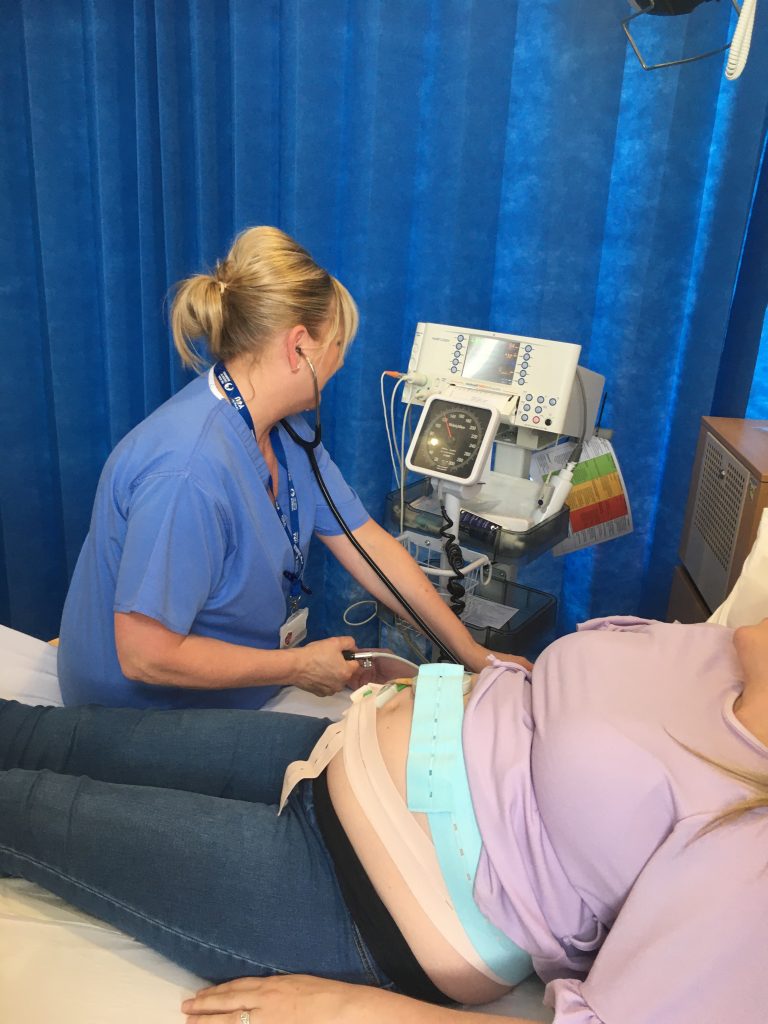
There are many changes to your baby’s heart rate and interpreting these changes is a highly skilled job. Throughout your labour if your baby’s heart rate is monitored by continuous CTG, there will be a regular review with another midwife (sometimes called Fresh Eyes/Fresh Review/Buddy) to ensure the CTG is being interpreted correctly and discuss whether any doctors input is required. This discussion should include you and your birth partner, taking into account your wishes.
With continuous CTG monitoring, your ability to move freely will be more limited, however you will still be encouraged to adopt upright positions. If it is available, CTG monitoring via a wireless telemetry CTG machine may be used to encourage mobility and also use in the birth pool.
Occasionally, there may be instances where the abdominal sensor is not sufficient enough to monitor your baby’s heartbeat and a fetal scalp electrode (sometimes called a scalp clip) may be offered and applied to your baby’s head. It is applied by performing a vaginal examination and the electrode picks up your baby’s heartbeat directly.
It is usually considered if there are concerns with the baby’s heartbeat and there are difficulties monitoring abdominally, or more routinely in the case of twin pregnancy or raised maternal Body Mass Index (BMI).
- Pain relief while having your baby
- Epidural (service available 24 hours per day)
- Hydrotherapy (pool)
- Simple analgesia (paracetamol)
- Entonox (gas and air)
- Diamorphine
- Pethidine
Within our delivery suite we aim to ensure that your birth experience is as normal and low key as possible with care provided by caring and efficient midwives.
However, we take into consideration your clinical needs and when further assistance is required, medical staff are present on the Maternity Unit 24 hours per day.
Therefore, whether you are having a normal birth, planned caesarean section or need either a forceps, ventouse or emergency caesarean section delivery, there is a full team of midwives, obstetricians and support workers available to provide your care.
- Visiting times
Within the maternity unit we believe in family centered care, but in order to allow for privacy to patients, rest periods for mums and babies, doctors rounds, medical examinations and to ensure security for mums and babies, visiting times will be restricted as follows:
Antenatal and postnatal wards
Birthing partners: 9am – 9pm
Visitors: 2pm – 4pm and 6pm – 8pm
Visitors are limited to three persons per bed.
Delivery suite
To ensure the maintenance of security and privacy for all patients on delivery suite there are no visiting hours on delivery suite. Access is allowed to the maximum of 2 birthing partners only.
Visitors are not allowed in theatre or the recovery room and the swapping of birthing partners during labour is not allowed.
Any other visitors will be advised to visit during allocated visiting hours on antenatal or postnatal wards following transfer of mum and baby.
Children
Only the brothers and sisters of the new-born should be brought in. Other children will not be allowed within the ward areas.
- Security
Keeping you and your family safe
All doors to the maternity wards are kept locked and only members of staff working within the maternity unit can gain entry via their identification badge. An intercom and security cameras are used to assess visitors before entry to the wards.
All babies are security tagged at birth as well as wearing their identification tags. However, you should never leave your baby unattended. If you need to leave your baby for any reason please inform the midwife.
If for any reason your baby’s identification tag comes off, please inform a midwife straight away.
We practice a “rooming in” policy which means that your baby will be cared for with you in attendance, therefore never let your baby be taken away by any one.
All staff wear an identification badge if you cannot see it, please ask.
For security reasons women and their visitors are requested not to let any one in to or out of the wards.
- Feeding your baby
During pregnancy you will be given the opportunity to talk about feeding your baby. This will include the benefits of breastfeeding for baby and for you, the value of skin contact, closeness, comfort and responding to your baby’s needs.
Being prepared about your chosen feeding method is of great benefit especially if you have chosen to breastfeed. Infant feeding information will be given and discussed with your midwife and in greater detail in our parent education programme.
We also have an infant feeding workshop which is held twice a month in Ormskirk hospital and will give you all the information and support to help you make your feeding decision.
 Call 01695 656502 to contact Lesley Fawcett, our infant feeding co-ordinator
Call 01695 656502 to contact Lesley Fawcett, our infant feeding co-ordinatorContact your community midwife to book on to parent education classes and for infant feeding workshop dates.
Breastfeeding Groups and Breastfeeding Peer Support
Visiting a breastfeeding group both during pregnancy and after your baby is born can be a great way to share experiences and meet with other breastfeeding mums.
Other organisations for breastfeeding support and information
National Childbirth Trust 0300 330 0700
National Breastfeeding Helpline 0300 100 0212
The Breastfeeding Network 0300 100 0210
Both lines are open between 9.30am – 9.30pm every day. Call to speak to trained volunteer mothers.
Leaflets
For the following leaflets – Off to the best start, Building a Happy Baby, Caring for your baby at night, Feeding twins, Expressing, Caring for your Premature baby, Formula feeding, Breastfeeding at study and work, responding to babies needs and more please follow this link
Videos
For videos on skin to skin, meeting baby for the first time, positioning and attachment, hand expressing, expressing and storing breastmilk, responsive feeding and relationship building and more please follow this link
Feeding your baby at nightime
For information and leaflets about feeding your baby safely at night time follow this link.
Breastfeeding out and about

You shouldn’t ever be made to feel uncomfortable about breastfeeding in public. It is illegal for anyone to ask a breastfeeding woman to leave a public place, such as a cafe, shop or public transport.
During your baby’s early days, you may prefer to breastfeed only where you feel most comfortable. But, as you get more used to doing it, you’re likely to feel more confident about breastfeeding in front of other people when you’re out and about.
There are a number of venues signing up to breastfeeding friendly schemes. Contact your local breastfeeding peer support service for a list of places near to you. Follow this link for more information on breastfeeding out and about.